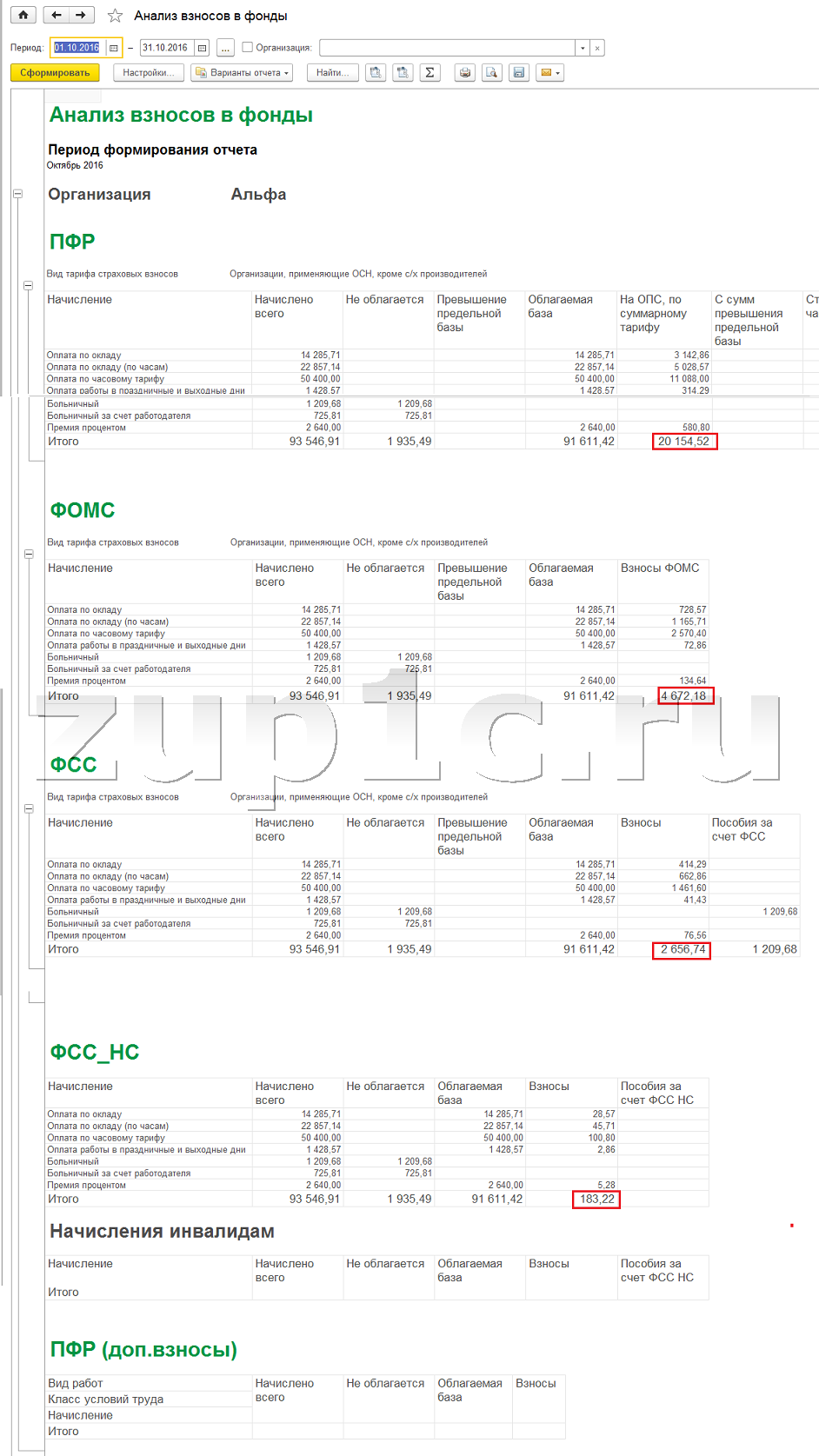
Rasshifrovka Kodov Raschetnogo Lista Shahtera
Pravoslavnye prazdniki svoej istoriej ukhodjat v davnie vremena Vetkhogo zaveta. Program alcormpufd untuk ic alcor au6986 1. Kazhdaja pamjatnaja data posvjaschena osobomu vospominaniju cheredujuschikhsja sobytij i chtimykh Svjatykh. Po vazhnosti sobytij prazdniki razdeljajutsja na velikie, srednie i malye, a po vremeni prazdnovanija - na podvizhnye ili perekhodjaschie i nepodvizhnye.
Natriuretic regulation of extracellular fluid volume homeostasis includes suppression of the renin-angiotensin-aldosterone system, pressure natriuresis, and reduced renal nerve activity, actions that concomitantly increase urinary Na + excretion and lead to increased urine volume. The resulting natriuresis-driven diuretic water loss is assumed to control the extracellular volume. Here, we have demonstrated that urine concentration, and therefore regulation of water conservation, is an important control system for urine formation and extracellular volume homeostasis in mice and humans across various levels of salt intake.
We observed that the renal concentration mechanism couples natriuresis with correspondent renal water reabsorption, limits natriuretic osmotic diuresis, and results in concurrent extracellular volume conservation and concentration of salt excreted into urine. This water-conserving mechanism of dietary salt excretion relies on urea transporter–driven urea recycling by the kidneys and on urea production by liver and skeletal muscle. The energy-intense nature of hepatic and extrahepatic urea osmolyte production for renal water conservation requires reprioritization of energy and substrate metabolism in liver and skeletal muscle, resulting in hepatic ketogenesis and glucocorticoid-driven muscle catabolism, which are prevented by increasing food intake. This natriuretic-ureotelic, water-conserving principle relies on metabolism-driven extracellular volume control and is regulated by concerted liver, muscle, and renal actions.
It has long been viewed that the maintenance of osmotic balance in response to high salt intake is a passive process that is mediated largely by increased water consumption to balance the salt load. Two studies in this issue of the JCI challenge this notion and demonstrate that osmotic balance in response to high salt intake involves a complex regulatory process that is influenced by hormone fluctuation, metabolism, food consumption, water intake, and renal salt and water excretion. Rakova et al. Report the unexpected observation that long-term high salt intake did not increase water consumption in humans but instead increased water retention. Moreover, salt and water balance was influenced by glucocorticoid and mineralocorticoid fluctuations. Kitada et al. Extend upon these findings in mouse models and determined that increased urea and a corresponding increase in urea transporters in the renal medulla as the result of increased protein intake promote the water retention that is needed to achieve osmotic homeostasis.
Together, the results of these two studies lay the groundwork for future studies to determine how, in the face of chronic changes in salt intake, humans maintain volume and osmotic homeostasis. The idea that increasing salt intake increases drinking and urine volume is widely accepted. We tested the hypothesis that an increase in salt intake of 6 g/d would change fluid balance in men living under ultra-long-term controlled conditions. Over the course of 2 separate space flight simulation studies of 105 and 205 days’ duration, we exposed 10 healthy men to 3 salt intake levels (12, 9, or 6 g/d). All other nutrients were maintained constant. We studied the effect of salt-driven changes in mineralocorticoid and glucocorticoid urinary excretion on day-to-day osmolyte and water balance. A 6-g/d increase in salt intake increased urine osmolyte excretion, but reduced free-water clearance, indicating endogenous free water accrual by urine concentration. 